Home » Health News »
Can an exhausted lung cell of a smoker fight bacterial infection?
Researchers at Trinity College Dublin have discovered how lung cell exhaustion affects a patient’s ability to fight diseases.
Their findings are published in the American Journal of Respiratory Cell and Molecular Biology.
What happens to the crucial immune cells in the lung of a smoker when they come into contact with bacterial infection?
Unfortunately not much. The lung cells, called macrophages, of a smoker are exhausted from their daily exposure to smoke, rendering them unable to do their job. They are no longer able to respond to the challenge set before them which is to kill infection. However, little is known about how smoking causes tuberculosis susceptibility.
Now scientists at Trinity College Dublin and St James’s Hospital have compared the lung cells of smokers to non-smokers to better understand how lung immunity against tuberculosis works. They are working to design ways to support the human immune system to prevent this infectious disease arising in marginalised members of society.
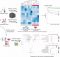
The scientists have shown that lung macrophages can turn on helpful pathways of energy production after infection with the tuberculosis bacteria. Using lung cells, kindly donated by volunteers who attend the hospital, they have now demonstrated that these energetic pathways can be recruited in the lung after bacterial infection. This can effectively control the bacteria after it has been inhaled from an infectious person with TB. This ability to switch metabolism appears to be a central process in host defence.
When the team looked at lung macrophages taken from volunteers who smoke, they noticed that these smokers’ cells had markedly reduced metabolic activity – and had no metabolic reserves to respond to the infection. This is a first description of smoker’s lung cells as an exhausted macrophage, and the investigators are now looking at ways to restore these helpful pathways to fortify immunity in smokers – to prevent infectious diseases.
Commenting on the significance of the finding, Research Fellow in Clinical Medicine at Trinity College Dublin, Dr. Laura Gleeson, who is a recipient of the HRB health professional fellowship, said “because volunteers attend St James’s and partake in medical research, we were able to tightly compare smokers to non-smokers – to understand better how lung immunity against tuberculosis works. Our new description of macrophage exhaustion in the lung might also lead to treatments that could be applied to other TB susceptible groups. These include persons who suffer from immunosuppressive conditions such as diabetes, HIV, and those taking immunosuppressive drugs.”
Source: Read Full Article