Home » Health News »
New vaccine concept against SARS-CoV-2 successfully tested
Researchers at the University of Basel have developed a new approach for a vaccine against COVID-19. This vaccine is based on a modified coronavirus that can enter body cells and trigger an effective immune response but cannot multiply in the body. In animal studies, the vaccine effectively protected against the disease and even prevented virus transmission. Clinical trials in humans are to follow.
Although safe and effective COVID-19 vaccines have been available since early 2021, SARS-CoV-2 continues to spread, with new variants continuously emerging. In some regions, the population lacks access to vaccines; in others, there is a lack of confidence in the novel mRNA vaccines. New vaccines that are easy to store and administer and that build up effective immune protection would be an important step toward keeping the SARS-CoV-2 coronavirus at bay in the long term.
Researchers led by Professor Thomas Klimkait of the Department of Biomedicine at the University of Basel, in collaboration with the company RocketVax, are now presenting a vaccine concept that could lead to a new generation of vaccines against SARS-CoV-2. This concept can also be rapidly adapted to new variants and even to other viruses. Their promising results are now being submitted to a peer-reviewed journal for publication and are accessible on the bioRxiv preprint server.
Vaccine virus incapable of replication
“Single-cycle virus” is how the researchers describe the principle of their novel vaccine. The vaccine is based on a specially adapted version of the virus that can be produced in the laboratory. In cells of the vaccinated person, however, the single-cycle virus cannot replicate further after the initial entry.
A virus normally brings with it, in its genetic material, the blueprints for all the components needed for new virus particles. Once inside a cell, the virus then misuses the cellular machinery—the cell begins to multiply the virus. Subsequently, newly built viruses destroy the cell and go on to infect other cells.
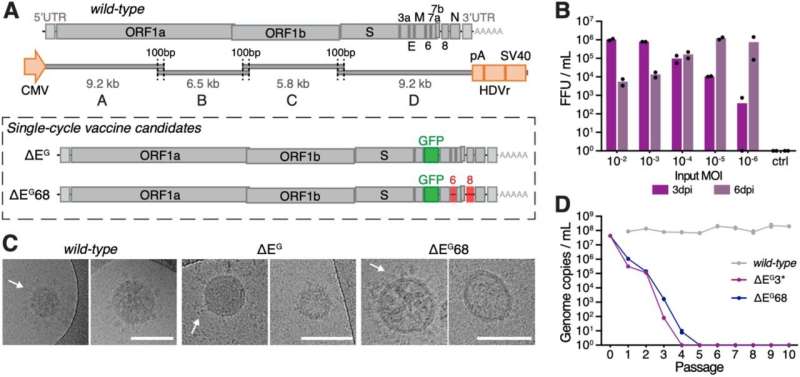
For their vaccine, however, the researchers modify the genome of the virus. “Among other things, we remove a specific gene from the blueprint for the viral envelope,” explains Klimkait, a virology expert. If this envelope component is missing, no new virus particles can be formed. Yet, the body cells still produce the remaining components of the virus and present them on their surface to the immune system, which recognizes the viral components and builds up effective immune protection.
Vaccine production using a special cell line
To ensure that the virus can still be made for vaccine production—given that it can no longer multiply in normal cells—the researchers developed a unique “production cell line.” They did this by incorporating the missing gene for the virus building block into the genetic material of special cells so that they now produce this component on a permanent basis. If the modified virus (with an incomplete blueprint for the viral envelope) is now used to infect these production cells, complete virus particles can efficiently be produced.
“Externally, these vaccine viruses are identical to normal coronaviruses. But a viral envelope gene is missing from their genome. This means that they cannot replicate in normal body cells, which have no substitute to offer,” says Dr. Christian Mittelholzer, the scientist leading this project.
Improved immune response
Apart from the missing blueprint for the viral envelope building block, the researchers altered other details of the viral genome—they removed genes that allow the virus to reduce the cells’ defense. These changes aim to enable a most effective immune response to the virus and to facilitate strong and long-lasting immune protection.
The researchers recently tested their new vaccine successfully in hamsters: After immunization administered by nasal drop, 20 out of 20 animals were protected: They developed no symptoms even after contact with a high dose of the natural SARS-CoV-2. Moreover, the vaccine was able to prevent transmission of SARS-CoV-2 to other, unvaccinated animals. Thus, according to current knowledge, they built up sterile immunity.
Vaccination without needles
For humans, the plan is also to administer the vaccination by nose or mouth. In addition, as the single-cycle virus is highly stable, the vaccine can simply be stored in the refrigerator for long periods of time, says Klimkait. The research team is now planning towards vaccine production and a human study with a small cohort of subjects in Switzerland.
Should new variants or even a “SARS-CoV-3” emerge, Klimkait explains that the same concept can be used and quickly adapted to the new virus. “From a technical point of view, we introduce the modified virus genome as several pieces into the production cell line, because that is easier to produce and sneak in.” Inside the cell, repair enzymes ensure that the pieces of virus genome are put back together to form a whole. “This also means, for example, that we can easily exchange the section containing the blueprint for the spike protein if a new variant emerges with new mutations,” says Klimkait.
It is impossible for the missing gene, corresponding to the viral envelope building block, to return, Klimkait emphasizes. “The envelope protein gene is located in the genetic material in the nucleus of the production cell. The virus genome, on the other hand, always remains outside the nucleus—so they never meet, and the virus genome cannot restore itself to the original version.”
More information:
Martin Joseph Lett et al, Single-cycle SARS-CoV-2 vaccine elicits high protection and sterilizing immunity in hamsters, bioRxiv (2023). DOI: 10.1101/2023.05.17.541127
Journal information:
bioRxiv
Source: Read Full Article



