Home » Health News »
Towards more effective treatments for immunocompromised patients
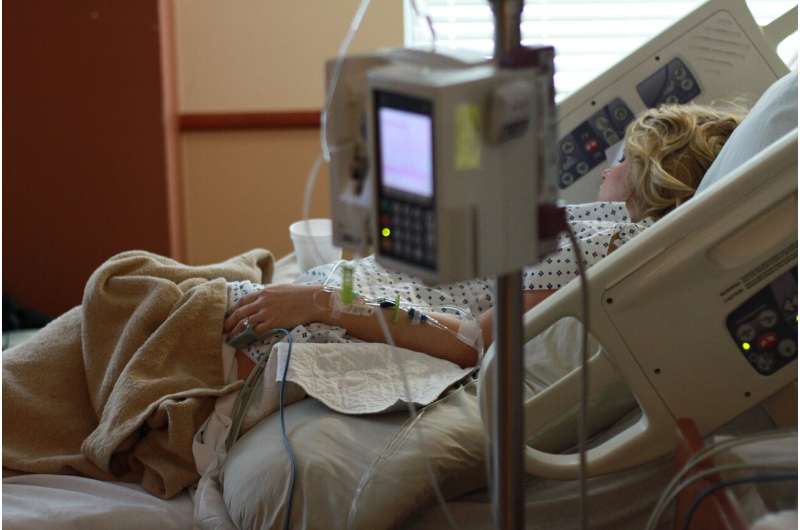
For severely immunocompromised patients, a bone marrow transplant restores immune defenses and allows them to resume normal life. But after observing the nasopharyngeal system, where the body’s first line of immune defense is deployed, scientists from the Institut Pasteur, Université Paris Cité, Inserm and the Paris Public Hospital Network (AP-HP), in collaboration with the Imagine Institute, demonstrated a failure in the immune mechanisms of some of these patients. The results of this study, published in the journal Blood on February 14, 2022, could pave the way for more effective treatment.
In patients with severe combined immunodeficiency (SCID), the immune system is compromised and unable to deal with the onslaught of microbial attacks from the environment. Alain Fischer, a founding member of the Imagine Institute at Necker-Enfants Malades Hospital (AP-HP), has followed these patients for the past 30 years and knows them well. “SCID patients need to be treated with an allogeneic bone marrow transplant, sometimes combined with pre-transplant chemotherapy to prevent graft rejection,” explains the physician and immunologist. “This procedure cures patients and restores their immune system, but we had never previously taken a detailed look at what was happening in the nasal mucosa.” The immune response machinery is highly complex and involves several components: agents in the innate immune response, which are particularly active in the mucosa of the gut, lungs and nose, and agents in the adaptive immune response, which circulate in the blood and lymph.
To help elucidate the way in which the innate immune system is regulated, James Di Santo, Head of the Innate Immunity Unit (Institut Pasteur/Inserm), proposed comparing the post-transplant immune systems of immunocompromised patients with the immune systems of healthy patients from the “Milieu Intérieur” cohort. “We already had nasopharyngeal samples taken with a simple nasal swab from some 1,000 subjects, and we were able to study the immune response using these samples,” says the scientist. “The idea was to take the same type of samples from immunocompromised patients, together with a blood test, to observe the differences.”
The scientists soon saw significant differences in some patients. Although in the healthy subjects and most of the immunocompromised patients the entire nasopharyngeal system had generally geared up to respond to attacks by forming a protective mucus layer, producing a large quantity of antibodies (especially IgA antibodies) and immune cells, and maintaining the microbiota, the nasal mucosa was disrupted in some transplant patients. In patients who were partially immunocompromised and had received only limited pre-transplant chemotherapy, the nasopharyngeal region had a smaller quantity of mucus, fewer IgA antibodies and cytokines and a prevalence of pathogenic bacteria. In other words, the mucosal immune system in these individuals was less active in dealing with daily attacks from pathogens. Their blood samples also revealed a selective deficiency in some circulating immune cells.
Source: Read Full Article


